In 2024, healthcare was captivated by AI that could generate language. In 2025, organizations began embedding tools that could listen and document. Now, in 2026, the industry is entering a more consequential phase: the deployment of sophisticated Agentic AI Use Cases.
These are not copilots offering suggestions on the sidelines. They are systems designed to execute clinical intent, coordinate actions across platforms, and carry tasks through to completion.
Let’s explore the Top 5 Agentic AI Use Cases in Healthcare Clinical Workflows with us. You will see where agents are already delivering measurable operational value, how they are reshaping documentation, decision support, care coordination, and population health.
Key takeaway
- Health system executives expect agentic AI to deliver moderate-to-significant value across clinical and operational functions in 2026.
- 2026 marks the transition from single-turn generative AI to multi-step Multi-Agent Orchestration.
- The five most transformative agentic AI use cases in clinical workflows span autonomous CDS, ambient documentation, care coordination, prior authorization, and population health.
How Agentic AI will transform healthcare in 2026
Unlike passive AI tools that respond when asked, agentic systems are goal-driven, autonomous, and capable of executing multi-step processes across disparate systems with minimal human intervention.
They perceive context, plan actions, use tools, validate outputs, and escalate when uncertain, much like a highly competent clinical coordinator who never sleeps.
The macroeconomic pressure to adopt is undeniable. U.S. health spending reached $4.9 trillion in 2023 and the 2024 CAQH Index identifies a $20 billion savings opportunity from automating routine administrative transactions alone.
Healthcare institutions allocate approximately 20% of their budgets to administrative tasks, while physicians dedicate roughly 25% of their working hours to documentation and administrative duties (PMC, 2025).
Something has to give, and agentic AI is increasingly the answer.
Multi-Agent Orchestration and Complex Workflows
The most powerful shift in 2026 is not any single AI agent.
It is the emergence of multi-agent ecosystems where specialized agents collaborate, delegate, and check each other’s work across complex clinical and administrative workflows. Think of it as a distributed intelligence layer running in parallel with your existing EHR infrastructure.
Read more: How Multi-Agent Orchestration Solves EHR Fragmentation in 2026
Autonomous AI agents are moving beyond pilot programs into full-scale healthcare deployment in 2026, with 68% of healthcare organizations already using agent-based systems and McKinsey projecting $80-$110 billion in annual cost savings for private payers alone.
This multi-agent architecture transforms what was a serial, human-driven workflow into a parallelized, intelligent operation. Several specialized agents intake, evidence retrieval, policy interpretation, clinical reasoning, communication and work in concert, completing in minutes what previously took hours of manual coordination.
Advancements in Drug Design and Post-Market Monitoring
Beyond the clinical encounter, agentic AI is reengineering how new therapies are discovered and monitored.
AI agent networks are increasingly being used to identify novel drug targets, repurpose existing molecules, and accelerate the early stages of the development pipeline.
The numbers are in, and they spell change for life sciences. That’s because nearly three-quarters (73%) of global pharmaceutical organizations are actively planning, piloting, or deploying agentic AI initiatives.
On the post-market front, agentic AI is redefining pharmacovigilance. These systems operate as persistent, autonomous monitors – continuously scanning adverse event databases, real-world evidence, and patient-reported outcomes for emerging safety signals.
Unlike traditional reviews that occur at fixed intervals, agentic surveillance never pauses. It detects patterns early, escalates risks proactively, and embeds intelligence directly into the pharmacological monitoring infrastructure.
Transformation of the Patient and Physician Relationship
The third and perhaps most humanistic dimension of agentic AI’s impact is how it is restoring the quality of the clinical encounter.
Physicians notice the impact of having their cognitive load lightened. We’re more focused throughout the day and less mentally exhausted, leaving more energy and compassion to dedicate to improving patients’ quality of life.
By absorbing the administrative and documentation burden that has long pulled clinicians’ attention away from patients, agentic AI is making space for something that algorithms can never replicate: genuine human presence.
Why Agentic AI is a Game-Changer in Clinical Workflows?
Transforming Documentation
For every hour a physician spends with a patient, they spend approximately 2 hours on documentation and EHR-related tasks. This ratio, often described as the “2:1 burden,” has driven burnout and contributed to clinical errors.
Agentic documentation systems, starting with ambient AI scribes and evolving into full clinical agents, are directly inverting this equation.
These agents don’t merely transcribe. They perceive conversational context, extract clinically relevant information, map it to structured EHR fields, suggest diagnostic codes, and flag potential documentation gaps. All while the encounter is still happening.
UW Health’s randomized trial, covering over 800 physicians across Wisconsin and Illinois, found that Agentic AI reduced documentation time by 30 minutes per day per provider and improved billing code accuracy. The system has since been rolled out system-wide.
Accelerating Clinical Decision-Making
Traditional clinical decision support generated alerts and clinicians learned to ignore them.
Alert fatigue became its own patient safety issue. Agentic CDS systems break this pattern by synthesizing patient data, literature, and real-world evidence to proactively deliver actionable, personalized guidance without waiting to be asked.
The shift from reactive alerting to proactive intelligence is one of the most clinically significant changes agentic AI enables in 2026. Four in ten healthcare executives already use AI for inpatient monitoring and early patient health warnings, an area expected to see full agentic implementation within three years.
Burnout Reduction
The burnout crisis isn’t a wellness metric – it’s an existential threat to care quality.
A JAMA Network Open study found that after 30 days with an ambient AI scribe, burnout among ambulatory clinic clinicians decreased significantly from 51.9% to 38.8%.
The administrative “tax” on medicine is finally being repealed.
Top 05 Agentic AI Use Cases in Healthcare Clinical Workflows
Autonomous Clinical Decision Support (CDS) Agents
These agents function as a “digital resident.” They don’t just wait for a query; they proactively scan the EHR for “care gaps” or contraindications.
Traditional rule-based CDS was blunt: it generated static alerts that clinicians clicked past thousands of times per day, generating noise rather than insight.
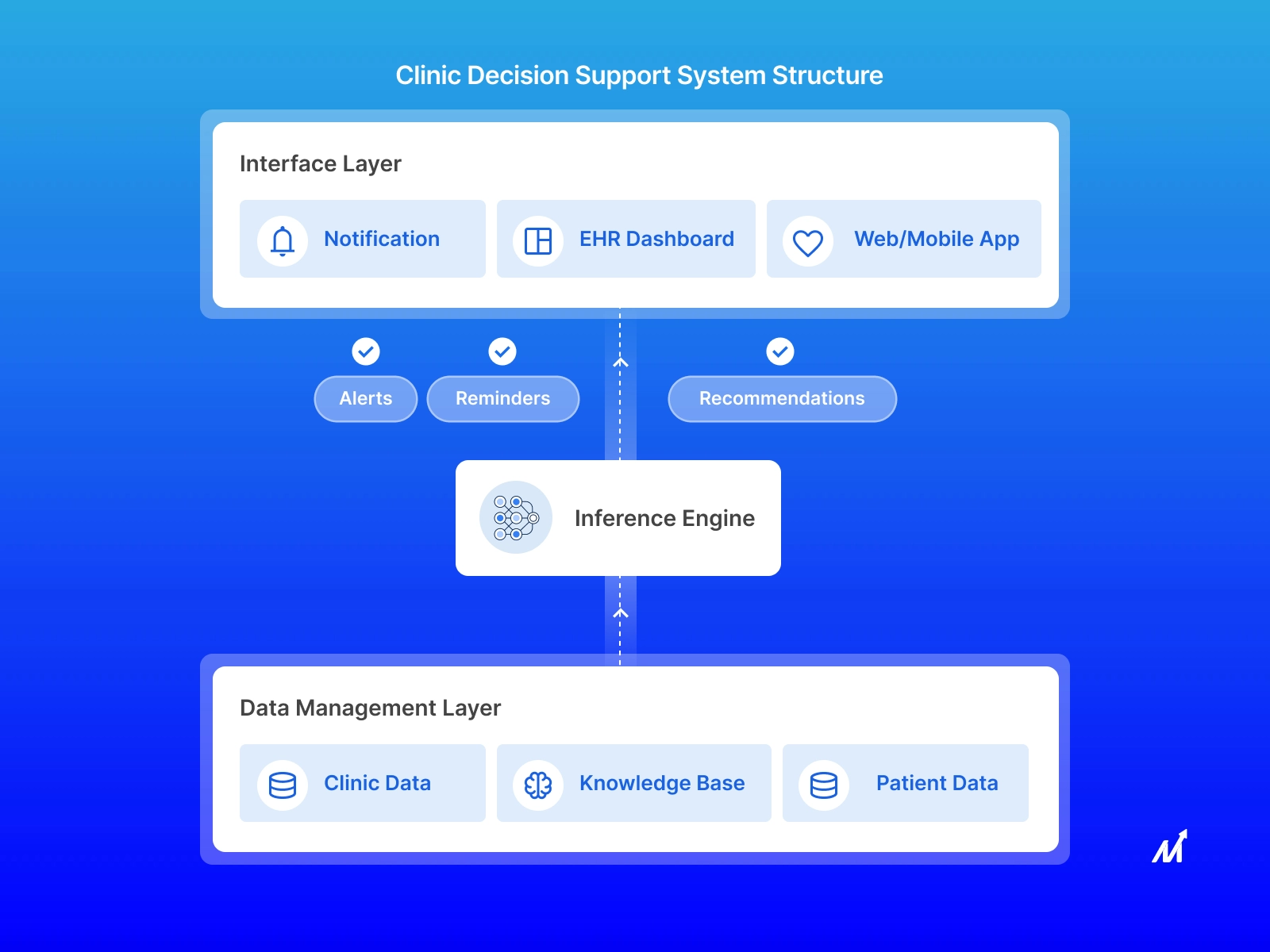
Clinical Decision Support System Structure (Source: Markovate)
Agentic CDS operates at a fundamentally different level. These systems continuously monitor real-time patient data streams, cross-reference evidence-based guidelines, consult longitudinal records, and surface timely, personalized recommendations – without being asked.
The healthcare industry has a high usage rate of AI agents at 68%, and 84% of survey respondents feel comfortable with AI making end-to-end autonomous decisions for specific processes.
60% of health system executives agree that agentic AI will meaningfully improve or disrupt the provider-patient experience, with similar optimism around productivity gains at 57%.
Ambient Clinical Documentation Evolving into Clinical Agents
Ambient AI scribes were the gateway drug for agentic AI in clinical settings. But in 2026, we are witnessing the evolution of ambient documentation into full-spectrum clinical agents, creating some of the most impactful Agentic AI use cases in healthcare.
Multi-site evidence from JAMA Network Open and NEJM AI shows ambient AI is delivering measurable impact: a 21.2% absolute reduction in burnout at Mass General Brigham, a 30.7% increase in documentation-related wellbeing at Emory Healthcare, and up to 30 minutes saved per clinician per day at UW Health.
The trend is clear: ambient documentation is evolving from passive transcription into proactive clinical agents that not only reduce workload, but increasingly structure data, trigger actions, and embed intelligence directly into care workflows.
All within a single workflow.
Multi-site evidence from JAMA Network Open and NEJM AI shows ambient AI is delivering measurable impact: a 21.2% absolute reduction in burnout at Mass General Brigham, a 30.7% increase in documentation-related wellbeing at Emory Healthcare, and up to 30 minutes saved per clinician per day at UW Health.
The trend is clear: ambient documentation is evolving from passive transcription into proactive clinical agents that not only reduce workload, but increasingly structure data, trigger actions, and embed intelligence directly into care workflows.
All within a single workflow.
Care Coordination and Discharge Planning Agents
Few clinical processes are as fragmented and high-stakes as discharge coordination. A typical discharge involves case managers, social workers, pharmacists, home health agencies, and transportation. Each is operating in silos and communicating via a cascade of phone calls and faxes.

The clinical stakes are severe: poor discharge coordination is a primary driver of preventable 30-day readmissions, costing the U.S. system billions annually.
Agentic AI replaces this fragmentation with a persistent, intelligent coordinator. These agents automatically schedule follow-up appointments, arrange home health services, update patient portals, send medication reminders, and flag early signs of post-discharge deterioration
All without provider intervention.
Deloitte’s 2026 Health Care Outlook identifies post-discharge monitoring pull-down a leading near-term agentic AI use case, with many organizations already piloting or deploying solutions. Health systems prioritizing discharge coordination report improved care continuity scores and reduced administrative workload for care management teams.
Multi-step follow-up workflows that once required dedicated staffing are increasingly automated through agent-driven orchestration.
The agent acts as the connective tissue of the post-acute care continuum, continuously operating long after the clinician has moved to the next patient.
Prior Authorization and Utilization Management Agents
Prior authorization is one of the most visible pain points in U.S. healthcare: a cost-control mechanism that has become a structural barrier to timely care.
Agentic prior authorization systems are beginning to remove one of healthcare’s most persistent bottlenecks at scale.
Unlike traditional RPA tools that simply automate form filling, agentic platforms interpret payer policies, adjust to real-time rule changes, analyze unstructured clinical documentation, and learn continuously from approval and denial patterns.
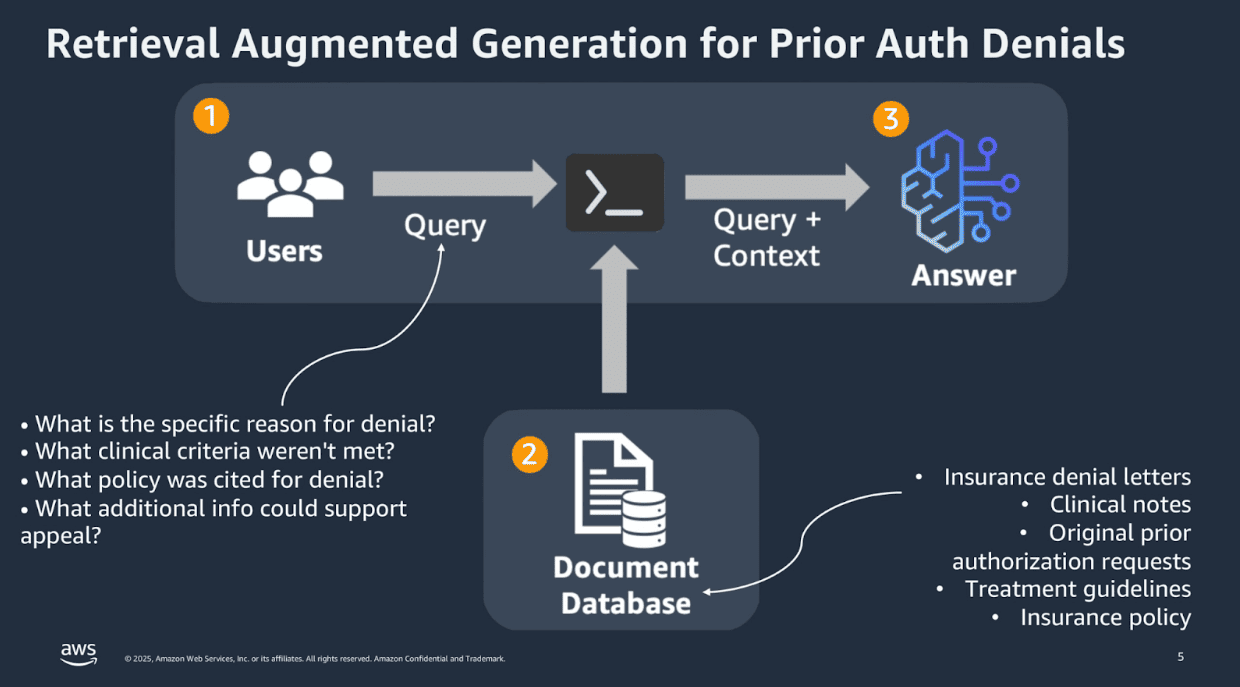
Through coordinated multi-agent architectures, the full prior authorization lifecycle moves in parallel, from intake validation and EHR data extraction to policy analysis, clinical reasoning, submission, tracking, and appeals.
What once required days of manual coordination can now be completed within hours, and in some cases, minutes.
Population Health and Care Gap Closure Agents
Managing the health of a population has always required something no human-staffed team could realistically deliver: continuous, personalized attention to every patient simultaneously. Traditional population health programs relied on periodic risk stratification and episodic outreach campaigns – a reactive model that missed patients until they escalated into high-cost episodes.
Agentic AI shifts the model from periodic to persistent. Intelligent agents continuously monitor preventive gaps, chronic disease indicators, medication adherence, and social risk signals across patient populations.
When an issue emerges, outreach is triggered automatically, whether through appointment prompts, reminders, or care team escalation. Population health moves from delayed response to always-on orchestration.
Future Outlook: Multi-Agent Ecosystems & Governance
As we look into the future of medicine, the strategic conversation is shifting from mere capability to robust governance. As these systems scale, “Governance as Code” will become foundational, ensuring that all Agentic AI Use Cases in Healthcare are observable, auditable, and accountable by design.
We are moving toward a sophisticated multi-agent ecosystem. For instance, one of the most transformative Agentic AI Use Cases in Healthcare involves a hospital discharge agent interacting in real-time with a payer authorization agent to coordinate logistics and approvals autonomously.
The primary constraint for these agents will not be technical sophistication, but organizational readiness. Sustainable success in deploying these Agentic AI Use Cases in Healthcare follows the 10-20-70 principle:
- 10% focus on algorithms.
- 20% on data architecture.
- 70% on people, workflow redesign, and operating model transformation.
Our team helps health systems assess readiness, design multi-agent architectures, and build governance models that earn clinician trust.
Contact us to schedule a strategic consultation





